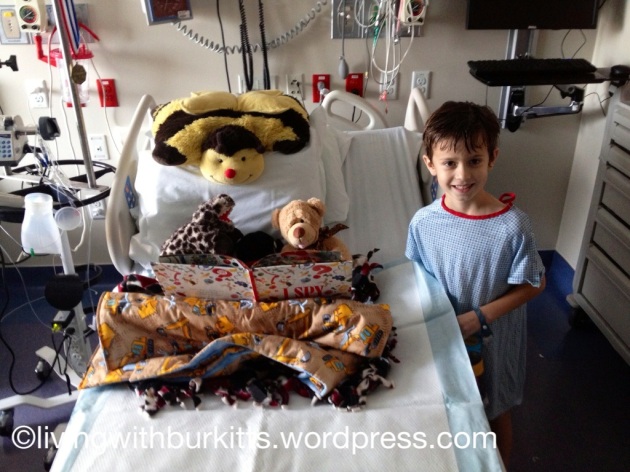
We have been overwhelmed with gratitude to everyone who has expressed their support in any way since Andrew has been in the hospital with what we now know is Burkitt’s Lymphoma. This has been the most difficult challenge of our lives. Wonderful family, friends, neighbors and colleagues have brought Andrew gifts, visited us at the hospital, sent cards, cared for Madeline, made Chris’ work days easier, taken over my PTA responsibilities, put up our Christmas decorations, bought us food, given us breaks, given us gift cards, cleaned our house, done our laundry, returned our library books, covered our home and street in yellow ribbons and even offered to be tested for bone marrow compatibility. It doesn’t look like that will be needed, but we are appreciative all the same.
Some of these acts of service occurred after we asked for help, while many others were done without our prior knowledge. Regardless of the reason, we are touched and humbled.It would be impossible for us to accept the offers of everyone who has offered to help in any way, but it is nice to know you’re there, because we have needed to accept some of those offers.
To those who are looking for ways to help us or families in a similar situation, here are some ideas.
1. Prayers and kind thoughts
We have felt gratitude for every person who has said or written that they are praying for us or thinking of us. It really does help just to know you care. To know that the powers of heaven are being called upon in our behalf by so many gives us great strength.
2. Gift cards
There will come a time when the home-cooked meals that have been offered will be needed and appreciated, but nobody has eaten more than cold cereal at our home in three weeks and counting. We have been doing lots of driving back and forth and paying for most of our meals in the cafeteria. When Chris’ co-workers gave us fuel and restaurant gift cards our first week here, it was the gift we would not have thought of on our own, but it was exactly what we needed.
3. Gifts and service to healthy siblings
Madeline doesn’t understand what Andrew is really going through, but she knows that he is receiving a lot of fun gifts and nearly all of her parents’ attention. It’s hard for healthy siblings not to feel frustrated and jealous. Grandma and Grandpa have been heroes for keeping Madeline’s life as normal and happy as possible. Neighbors have helped to pick her up from school and drive her to lessons and activities. If you’re thinking of gifts for a family with a sick child, consider the needs of healthy siblings as well.
4. Donations to the hospital
I have been amazed by how much we have benefitted from the donations of strangers to Primary Children’s Medical Center. We have played with the hospital’s toys, read its books, watched its DVDs and played its video games. Volunteers play live music in the lobbies and staff the playroom. Andrew has received new books and toys as gifts from the hospital and its donors. One of our friends makes hats for the cancer clinic. When she told us that, we had no idea how relevant it would be. PCMC is an amazing place and much of that is due to the generosity of many in the community.
We consider a donation to Primary Children’s Medical Center to be a donation to us. Here is a link where you can learn more about donating money or items to this special place. The Festival of Trees is happening in Sandy, Utah now. Be there. It’s a fun family event that supports Primary Children’s Medical Center.
5. Whatever feels right to you
Every gift has been appreciated because of the love with which it was given. The combined efforts of and ideas of many have staved off boredom and increased our comfort during some really long days. Visitors have brought fresh energy and smiles. Acts of service have brought grateful tears to our eyes. Toys, books, magazines, snacks, movies, cards, kids’ drawings, posters and more have lifted our spirits tremendously. Thank you. Thank you. Thank you all.
I have been taught how to be kind from so many of you. When this trial is behind us, I hope never to forget your example so that I can extend the same kindness to others.

Festival of Trees